Healthcare marketing used to be treated like a support function. That framing is outdated. In a market where patients compare providers online, expect faster access, read reviews before booking, and judge digital experiences long before they meet a clinician, healthcare marketing now shapes demand, trust, and revenue at the same time.
That shift is not just a branding story. It sits on top of real changes in patient behavior and healthcare operations. Recent research from Deloitte’s 2024 survey of more than 2,000 U.S. consumers, Press Ganey’s patient experience analysis based on 6.5 million encounters, McKinsey’s 2024 consumer health work, and Edelman’s 2024 Trust and Health report points in the same direction: people want care that feels easier to find, easier to understand, and easier to trust.
That is why healthcare marketing cannot be reduced to campaigns, slogans, or ad spend. Done well, it connects brand, reputation, patient experience, access, privacy, provider alignment, and measurable growth. Done badly, it creates demand that operations cannot absorb, weakens credibility, and increases compliance risk right when trust is hardest to earn.
Article Outline
- Why Healthcare Marketing Matters Now
- The Healthcare Marketing Framework
- Build Trust Before Demand
- Create Frictionless Access Across Channels
- Measure What Improves Growth and Experience
- Put It Into Practice Responsibly
Why Healthcare Marketing Matters Now
The biggest reason healthcare marketing matters more today is that patient choice has become more active and more digital. Research highlighted by Press Ganey’s work on provider reviews shows that reviews are not a side signal anymore; they are a core part of how patients evaluate clinicians and health systems. At the same time, Becker’s coverage of Press Ganey consumer findings reported that four in five consumers said online scheduling influences provider choice, which tells you something simple but important: access is now part of marketing.
That has strategic consequences. A hospital or practice can spend heavily on awareness and still lose patients if the website is confusing, reviews are thin, wait times feel opaque, or the next step after interest is unclear. Healthcare marketing is no longer just about getting attention; it is about turning attention into confident action.
Trust is the other force making this category more important. Edelman’s 2024 Trust and Health report found widespread concern about misinformation and the politicization of medical science, while Deloitte’s 2024 AI and health information research showed rising skepticism toward AI-generated health information. In practice, that means healthcare marketing has to do more than persuade. It has to reduce uncertainty, present evidence clearly, and make the organization feel credible before a patient ever submits a form or calls a location.
Operational pressure adds another layer. Press Ganey’s 2024 patient experience report shows that experience scores are improving in some settings, but the broader care journey still depends heavily on communication, responsiveness, and coordination. Marketing teams sit closer to those moments than many executives realize, because the promises made in search results, provider pages, service-line campaigns, and appointment flows directly shape whether the actual experience feels trustworthy or frustrating.

The Healthcare Marketing Framework
A practical way to think about healthcare marketing is to stop viewing it as promotion and start viewing it as a system. The strongest teams operate across four connected layers: market understanding, trust creation, access design, and performance improvement. That is the framework the rest of this article will use, because it reflects how modern healthcare decisions are really made.
The first layer is market understanding. You need to know which audiences matter most, what they are trying to solve, how they search, what barriers slow them down, and where your organization genuinely has an advantage. McKinsey’s healthcare consumer research and PwC’s digital patient experience perspective both reinforce the same idea: patient expectations are increasingly shaped by better digital experiences everywhere else.
The second layer is trust creation. In healthcare, trust is built through clarity, proof, consistency, and visible expertise. That includes reputation management, physician profiles, patient education, review strategy, quality signals, and careful communication across every touchpoint where a patient is deciding whether to move forward.
The third layer is access design. This is where many organizations still underperform. If a patient cannot quickly find the right service, understand the next step, verify insurance relevance, book online, or contact the right team without friction, the marketing system breaks even when campaign metrics look healthy. Deloitte’s 2024 virtual health findings and Press Ganey’s consumer experience analysis both point to convenience, responsiveness, and digital accessibility as major drivers of consumer choice.
The fourth layer is performance improvement. Healthcare marketing should be measured by business outcomes and patient-centered outcomes together, not by vanity metrics in isolation. That means connecting channel performance to appointment conversion, leakage reduction, service-line growth, provider utilization, review velocity, patient acquisition cost, and experience signals that show whether growth is actually sustainable.
One more point matters here, and it matters a lot: healthcare marketing operates inside a stricter privacy environment than most industries. The HHS guidance on online tracking technologies under HIPAA and the FTC’s updated Health Breach Notification Rule guidance make it clear that digital growth tactics cannot be separated from data governance. In other words, the best framework is not just growth-oriented. It is growth-oriented, operationally realistic, and compliance-aware from the beginning.

The rest of this article builds on that foundation. Next, we will look at the first real lever that makes healthcare marketing work in the real world: building trust before demand, not after it.
Build Trust Before Demand
The next mistake in healthcare marketing is assuming demand comes first and trust comes later. It does not work that way anymore. Patients usually meet your brand through search results, review platforms, provider profiles, location pages, referral conversations, health plan directories, and educational content long before they speak to a real person.
That means the trust layer has to be built before the campaign layer. If the first digital impression feels vague, outdated, overly promotional, or hard to verify, the patient does not experience your marketing as helpful. They experience it as risk.
This is where many organizations quietly lose growth. Not because the service is weak, but because the signals that should make the service feel credible are scattered across too many channels and managed too inconsistently.
Reputation Is the First Conversion Layer
Reputation management is often treated like a defensive task, but in healthcare marketing it is one of the clearest growth levers. Press Ganey’s research on provider reviews makes the point bluntly: patient reviews now sit at the center of the care discovery journey, and they shape trust before a visit ever happens through its 2024 analysis of provider review behavior. That is not a branding detail. It is conversion infrastructure.
The important shift is that ratings alone are not enough. Patients read language, patterns, recency, and response behavior. A profile with a strong star rating but stale reviews, sparse detail, or obvious friction around scheduling can still create doubt, especially when the care decision feels high stakes.
That is why healthcare marketing teams need a reputation system, not a review campaign. The system should cover review generation, location-level ownership, provider-level visibility, response standards, escalation rules, and recurring reporting tied to actual appointment demand. When reputation is managed this way, it stops being a vanity metric and starts acting like a trust engine.
Provider Profiles Do More Work Than Most Teams Realize
A lot of healthcare organizations still treat physician and clinician bios like static web copy. Patients do not. A 2024 survey of 543 consumers from Aha Media Group found that 92% read a doctor’s bio before booking an appointment, which is one of the clearest signals that the provider profile is not filler content. It is decision content.
That changes how healthcare marketing should approach these pages. A good profile does more than summarize credentials. It helps a patient quickly answer practical questions: does this clinician treat people like me, explain things clearly, align with my needs, accept my insurance context, and feel like someone I can trust with an important problem.
This is also where weak brand messaging gets exposed. Broad statements about compassionate care do very little if the individual provider pages are thin, generic, or hard to navigate. In practice, the provider profile often carries more persuasive weight than the homepage because it sits closer to the booking decision.
Helpful Content Builds Confidence Faster Than Promotion
Healthcare content works best when it reduces uncertainty. That sounds obvious, but a lot of content programs still chase traffic while ignoring the emotional reality of healthcare decisions. Patients are not just looking for information. They are trying to understand symptoms, options, urgency, treatment paths, and what the first appointment will actually feel like.
This is where trust and clarity intersect. The most effective healthcare marketing content does not sound like a campaign stretched into article form. It sounds like a competent guide that respects the reader, explains without exaggerating, and makes the next step feel manageable.
That matters even more in an environment shaped by misinformation and low confidence in many information channels. Edelman’s 2024 health trust research shows how fragile public confidence can be when people are surrounded by conflicting medical claims, and why trustworthy communication still has an outsized effect on behavior through its Trust and Health special report. In plain terms, healthcare marketing earns more by being useful than by being louder.
Privacy Is Part of Trust, Not Just Compliance
Patients do not separate privacy from brand credibility nearly as much as internal teams do. If a healthcare organization looks careless with forms, tracking, chat tools, or follow-up systems, the damage is not limited to legal exposure. It affects trust at the exact moment the patient is deciding whether to share personal information.
That is why privacy has to be designed into the marketing stack from the start. The latest HHS guidance on online tracking technologies and HIPAA and the FTC’s updated Health Breach Notification Rule materials make the broader point clear: healthcare growth teams cannot copy generic martech playbooks and assume they will be safe in a health context.
This has practical implications for every team building modern patient journeys. Forms, analytics, remarketing, chat experiences, CRM workflows, and automated messaging all need tighter governance than they would in a normal ecommerce funnel. Trust in healthcare marketing is not only what you say in public. It is also what your systems imply in private.
Trust Has to Feel Consistent Across Every Touchpoint
Patients do not judge your organization one channel at a time. They assemble a trust impression across all of them. A polished service-line page cannot compensate for inconsistent provider data, weak directory listings, poor reviews, hard-to-reach phone lines, or a booking path that breaks once real intent appears.
This is why the strongest healthcare marketing teams obsess over continuity. The language on the ad, the promise on the landing page, the provider profile, the insurance information, the appointment request flow, the confirmation message, and the follow-up all need to feel like they come from the same organization with the same level of care.
When that continuity is missing, performance problems usually show up downstream as lower conversion, higher leakage, weaker reviews, and poor referral retention. When it is present, trust compounds. The patient feels less friction, the organization feels more credible, and the next step becomes easier to take.
That leads directly into the next part of the playbook. Once trust is established, healthcare marketing has to make access feel simple, fast, and obvious, because credibility without convenience still leaves growth on the table.
Create Frictionless Access Across Channels
Once trust is established, the next job of healthcare marketing is to make action feel easy. This is where a lot of organizations underperform, because they still treat access as an operational issue that starts after marketing has done its part. In reality, the patient experiences access as part of the brand from the very first click.
That matters because intent in healthcare is fragile. A patient may be ready to book, call, or request care, but that motivation can disappear fast when the path is confusing, slow, or inconsistent. Recent consumer research summarized by Press Ganey and Becker’s Hospital Review shows how strongly online scheduling influences provider choice, which means convenience is no longer a nice feature around the edges of healthcare marketing. It is part of the core offer.
The Digital Front Door Has to Work Like a Real Front Door
The phrase digital front door gets overused, but the underlying idea is still important. Patients want one connected path from discovery to appointment, not a patchwork of provider listings, stale pages, call-center dead ends, and disconnected forms. Work from Deloitte on virtual and digital care demand, Kyruus Health’s 2024 patient access benchmark, and Healthgrades on healthcare consumer expectations all point to the same reality: patients increasingly expect healthcare access to feel as navigable as other modern service experiences.
That expectation changes the role of healthcare marketing. The website is not just a brand property. Service-line pages are not just SEO assets. Provider finders are not just directories. Together, they form the front door patients use to decide whether your organization feels easy enough to engage.
When the front door works, the patient feels momentum. They can identify the right location, the right clinician, the right next step, and the right contact path without second-guessing every move. When it fails, the organization pays for awareness but loses the conversion at the exact moment of intent.
Channel Consistency Matters More Than Channel Volume
A common mistake is expanding channel count before tightening channel consistency. More campaigns, more landing pages, more paid search groups, more social posts, and more listings do not automatically create better healthcare marketing. They often create more opportunities for conflicting information.
Patients notice inconsistency faster than teams expect. If paid search mentions same-day appointments, but the landing page makes availability unclear, trust drops. If a provider is listed under a specialty on one page and described differently on another, the path feels uncertain. If the location page, Google Business Profile, and scheduling flow do not line up, the friction becomes visible.
That is why the operational side of marketing has to be disciplined. Accurate provider data, service taxonomy, insurance language, call routing, location details, and appointment options all have to align. Kyruus Health’s benchmark research on access strategy emphasizes centralized provider data and stronger digital capabilities for exactly this reason through its 2024 benchmark report.
Access Design Should Follow a Clear Execution Process
This is the point where healthcare marketing becomes tangible. If a team wants to improve growth without creating more chaos, the execution process needs to be simple enough to follow and strict enough to enforce.
A practical access design process usually looks like this:
- Map the highest-value patient journeys by service line.
- Identify the exact points where users drop off, hesitate, or switch channels.
- Standardize the information needed to move forward with confidence.
- Reduce unnecessary steps between intent and booking.
- Connect follow-up workflows so no qualified inquiry disappears.
- Review performance monthly with both marketing and access teams at the table.
That sounds straightforward, but most organizations skip at least one of those steps. They launch campaigns before the booking path is stable. They improve page traffic without verifying that phone, form, and scheduling workflows are actually equipped to handle demand. Or they separate analytics from operations so completely that nobody can see where real losses are happening.
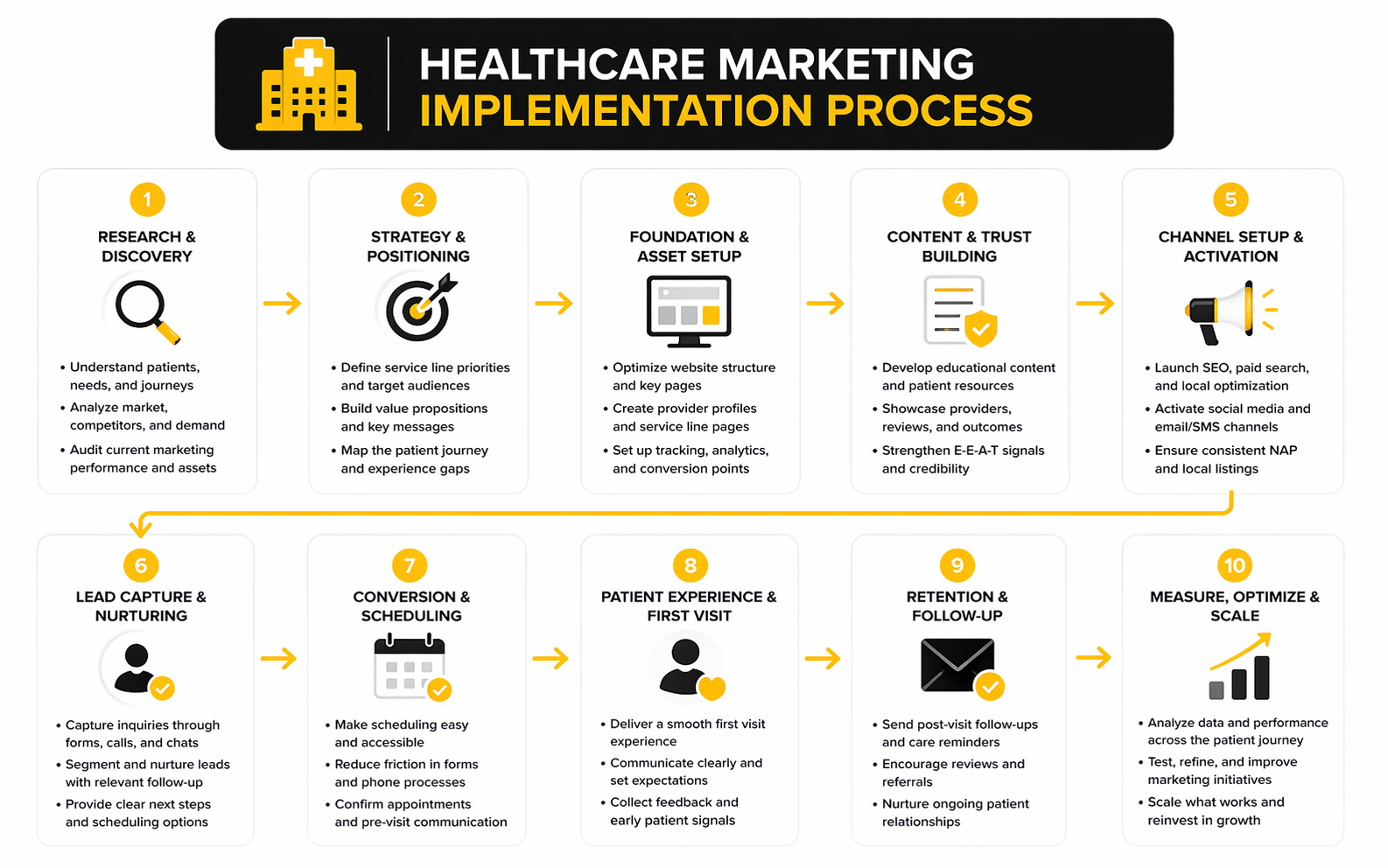
The better approach is to build healthcare marketing around journey design, not just campaign design. Start with the service lines that matter most financially or strategically. Then pressure-test every step from search result to confirmation message until the path feels obvious to a first-time patient, not just to the internal team that already understands the system.
Online Scheduling Is Only One Piece of the Process
Online scheduling matters a lot, but it is not the whole answer. Some services are too complex for instant booking. Some patients want reassurance before they commit. Some specialties need triage, referral context, insurance clarification, or prep instructions before an appointment makes sense.
That means healthcare marketing should offer multiple low-friction next steps instead of forcing every person into the same path. For one service line, that may be direct scheduling. For another, it may be a guided request form. For another, it may be a call route designed around urgency or complexity. The point is not to make everything uniform. The point is to make every path feel intentional.
This is where digital orchestration starts to matter. A system that combines structured forms, automated follow-up, simple routing, and calendar logic can tighten the gap between interest and response. Platforms built for workflow and lead handling, such as GoHighLevel, can be useful in adjacent service businesses, but healthcare organizations need to evaluate any stack through privacy, security, and operational fit before adopting it. In healthcare marketing, speed is useful only when it does not create new compliance or experience problems.
Messaging Has to Support the Next Step
A lot of conversion issues are actually messaging issues in disguise. The patient does not abandon because they are uninterested. They abandon because the next step feels uncertain, too early, too complicated, or mismatched to what they expected.
That is why strong access design depends on tighter message discipline. A page should explain who the service is for, what problems it addresses, what happens next, and how to proceed. A provider profile should reduce hesitation, not create more questions. A form should ask only what is necessary for the next action, not everything the organization might like to know eventually.
McKinsey’s recent work on healthcare consumer experience and AI-enabled engagement points toward the broader lesson through its 2024 healthcare consumer experience analysis. Personalization and smarter engagement can improve performance, but only if the underlying journey is already clear. There is no technology shortcut for a confusing offer.
Internal Alignment Is What Makes the Process Hold
This is the unglamorous part, but it is the part that keeps results from collapsing after one strong quarter. Healthcare marketing, patient access, operations, compliance, IT, and clinical leadership all shape the real patient journey whether they admit it or not. If those groups are working from different assumptions, the process starts leaking immediately.
The strongest teams create shared definitions for lead quality, scheduling readiness, response time expectations, provider data ownership, and channel escalation. They do not leave marketing to guess what operations can absorb. They do not leave access teams blind to what campaigns are promising. They do not wait for complaints to reveal system failures.
That kind of alignment is what turns healthcare marketing from activity into infrastructure. It makes growth more predictable because the organization is not improvising every time demand increases. And it sets up the next question the right way: once access is smoother and trust is stronger, how do you measure what is actually moving the business forward?
Measure What Improves Growth and Experience
Healthcare marketing gets expensive when teams measure attention instead of progress. Traffic can rise, impressions can look healthy, and lead volume can even increase while the real business stays flat because patients are dropping out between discovery, trust, and access. That is why measurement in healthcare marketing has to connect marketing activity to patient action, operational follow-through, and experience quality at the same time.
The useful question is not whether a campaign performed. The useful question is whether it improved the path from interest to care without creating more friction, more leakage, or more patient dissatisfaction. Once you start measuring that way, the numbers stop being decorative and start becoming operational.
The Metrics That Actually Matter
Most healthcare organizations already track channel metrics. The problem is that channel metrics alone rarely explain business performance. Click-through rate, cost per click, and pageviews can tell you whether attention is being captured, but they do not tell you whether the patient found the right provider, trusted the next step, or completed the booking path.
The more useful measurement stack starts with a handful of connected signals. These usually include branded and non-branded search demand, provider profile engagement, appointment conversion rate, call connection rate, online scheduling completion, no-show rate, review velocity, review sentiment, and new-patient acquisition by service line. Vizient’s 2024 ambulatory access compendium points to operational metrics like appointment lag, schedule optimization, and no-show performance as essential benchmarks, while Kyruus Health’s 2024 benchmark report ties digital access performance directly to acquisition and self-service outcomes.
This matters because healthcare marketing does not live in a clean ecommerce funnel. A patient may begin with search, move to a provider profile, leave to read reviews, return through a map listing, call instead of book, and schedule days later after checking insurance or speaking with family. If your analytics model cannot connect those behaviors, you will overvalue top-of-funnel activity and undervalue the assets that actually create confidence.
How to Read the Most Important Benchmarks
A strong benchmark only matters if you know what it is diagnosing. Take online access as an example. Federal health IT data show that in 2024, 77% of individuals were offered online access to their medical records, and patient portal use rose sharply when providers actively encouraged adoption, with 87% of encouraged patients accessing their portal at least once compared with 57% of those not encouraged. That does not just say digital access is growing. It says adoption depends heavily on how clearly the organization presents the next step.
The same logic applies to provider data accuracy. Kyruus Health reported that 30% of consumers delayed or skipped care after encountering inaccurate provider information in health plan transparency tools. That number should not be treated as a generic consumer stat. It should be read as a warning that directory quality, provider data governance, and listing accuracy are not side issues in healthcare marketing. They are conversion issues with direct care consequences.
Review behavior works the same way. Aha Media Group’s 2024 study found that 92% of patients read a provider bio before booking, and more recent consumer reporting in 2025 shows that online reviews remain a major decision factor when patients choose physicians. The practical meaning is simple: if profile engagement is high but appointment conversion is weak, the problem may not be awareness. It may be weak proof, weak profile quality, poor alignment between listing and landing page, or friction in the handoff to scheduling.
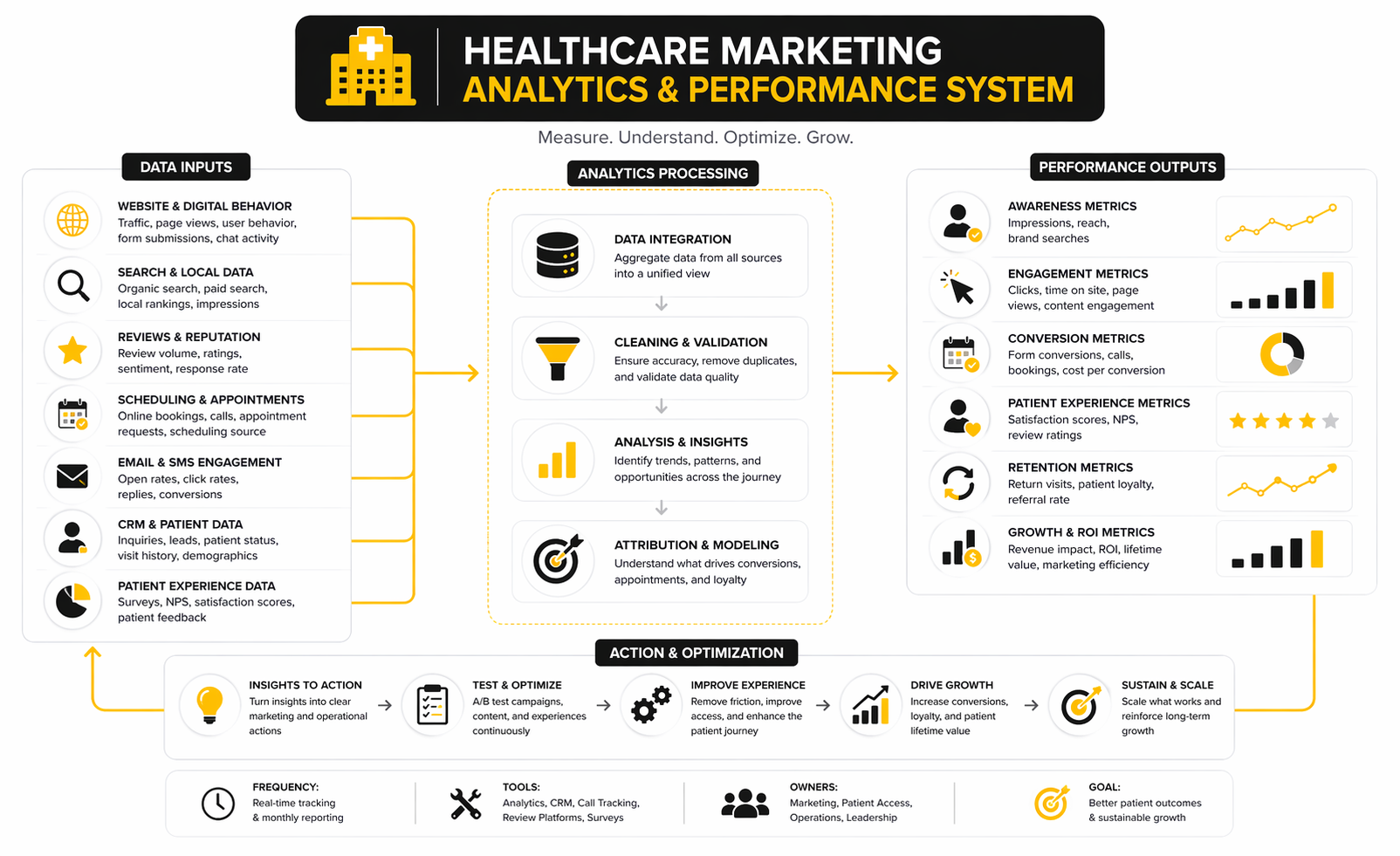
Build an Analytics System, Not a Dashboard Graveyard
A lot of healthcare organizations have data everywhere and clarity nowhere. One team owns paid media reports, another owns call-center reports, another owns web analytics, another owns patient access KPIs, and none of them line up cleanly enough to explain why growth is stalling. That is how dashboards multiply while accountability disappears.
A better system starts by measuring the journey in stages. One layer tracks visibility through search demand, listing impressions, and provider discovery. The next tracks confidence through profile engagement, reviews, content consumption, and abandonment on key pages. The third tracks action through calls, form completions, online scheduling starts, online scheduling completions, and booked appointments. The fourth tracks quality of growth through show rates, downstream utilization, patient experience, and reputation changes after the encounter.
That structure changes what the data can tell you. If visibility is strong but confidence is weak, the issue is probably trust or clarity. If confidence is strong but action is weak, the access flow is probably broken. If action is strong but quality of growth is weak, operations may be absorbing the wrong demand, or the experience after booking may be undercutting long-term value. That is the kind of interpretation healthcare marketing teams actually need.
What the Numbers Should Drive You to Do
Data should trigger action, not admiration. If provider pages attract traffic but few patients move forward, rewrite the profiles, improve the service taxonomy, tighten insurance language, and make next steps clearer. If listings traffic is healthy but patients abandon after landing, fix the continuity between the promise made in search and the experience delivered on the page.
If scheduling starts are high but completions are low, that usually points to workflow friction rather than weak demand. The remedy is often simpler than teams expect: fewer required fields, cleaner specialty routing, clearer visit-type language, and better fallback options when instant booking is not possible. Press Ganey’s work on consumer experience and online appointment scheduling reinforces the broader pattern that convenience has become a deciding factor, not a bonus.
If experience scores and reviews weaken after a marketing push, do not assume the campaign failed. It may have succeeded too well for the current operating model. Press Ganey’s 2024 report, based on 6.5 million encounters, is useful here because it highlights how communication, responsiveness, and the broader care journey continue to shape patient experience outcomes even when organizations improve in other areas. Growth that overwhelms access or communication quality is not healthy growth.
Use Benchmarks as Direction, Not as a Substitute for Judgment
Benchmarking matters, but it can mislead teams when it becomes lazy comparison. A multispecialty health system, a local orthopedic group, and an academic medical center should not expect identical conversion patterns, access behavior, or content engagement. The right benchmark is the one that helps you interpret progress in your own operating context while staying honest about what the market now expects.
That is why external data should be used to sharpen internal questions. If national data show patients are using portals, digital tools, reviews, and provider profiles more aggressively, the right response is not to chase every industry trend. The right response is to ask where your current patient journey still feels slow, unclear, or untrustworthy compared with those rising expectations.
At that point, healthcare marketing starts behaving like a management discipline instead of a campaign department. The numbers tell you where demand is building, where trust is holding, where access is breaking, and whether growth is actually improving the patient experience. That sets up the next step naturally: turning all of this into a working operating model that teams can sustain in the real world.
Put It Into Practice Responsibly
This is the point where healthcare marketing stops looking simple. Once the basics are working, the real challenge is not launching more campaigns. It is scaling growth without damaging trust, overloading operations, weakening compliance, or creating a patient experience that feels efficient on paper and frustrating in reality.
That is why mature healthcare marketing teams think in tradeoffs, not just tactics. Every growth move has a second-order effect. More demand can strain scheduling. More automation can make communication feel colder. More personalization can create governance risk if the underlying data and permissions are not tightly controlled.
Growth Gets Harder When Capacity Is Uneven
One of the biggest scaling problems in healthcare marketing is uneven capacity across service lines, locations, and providers. A campaign can look successful in the dashboard while quietly sending patients into long waits, limited appointment inventory, or overloaded contact centers. When that happens, marketing may still generate leads, but the organization starts burning trust faster than it builds demand.
This is where strategic discipline matters. Not every service line should be marketed with the same intensity at the same time. The better approach is to align promotion with actual access capacity, strategic margin priorities, and patient need so growth feels sustainable instead of chaotic.
That sounds obvious, but it is often ignored because campaign planning is easier than operational alignment. The problem is that patients do not care which department caused the friction. They only remember that the brand made a promise the system could not keep.
AI Can Improve the Journey, but It Also Raises the Stakes
AI is moving into healthcare marketing whether teams feel ready or not. It can help with segmentation, content operations, call routing, workflow support, conversational experiences, and faster internal analysis. Used carefully, that can make the patient journey more responsive and reduce some of the manual drag that slows good teams down.
But this is exactly where bad judgment gets expensive. Healthcare marketing cannot treat AI like a generic productivity layer and hope governance catches up later. If automated systems create misleading content, over-personalize in sensitive contexts, or handle patient information carelessly, the damage is not just technical. It is reputational, operational, and potentially legal.
The smarter approach is narrow and controlled. Use AI where it improves clarity, speed, and staff efficiency without pretending it can replace clinical authority, privacy controls, or human review. In other words, use it as an amplifier inside a governed system, not as a shortcut around one.
Attribution in Healthcare Is Always Messier Than Teams Want
Another advanced mistake is expecting perfect attribution. Healthcare decisions are rarely linear. A patient might hear about a provider from a friend, search the brand later, compare reviews, read educational content, call a location, postpone the decision, then finally book after a second search weeks later. No clean last-click model can fully represent that reality.
That does not mean attribution is useless. It means healthcare marketing has to combine directional channel data with journey-level interpretation and business context. Teams that demand impossible precision often end up making worse decisions because they underinvest in trust-building assets that influence choice but do not capture clean credit.
This is especially true for service lines with longer consideration windows, higher emotional stakes, or stronger referral interplay. In those cases, the goal is not to force false certainty into the reporting. The goal is to understand enough about contribution, sequence, and downstream performance to make better allocation decisions over time.
Brand and Performance Should Not Be Managed as Enemies
A lot of organizations still separate brand marketing and performance marketing like they belong to different worlds. In healthcare, that split causes real damage. Brand shapes trust, recall, and perceived credibility. Performance channels capture the intent that brand and reputation helped create. Break that connection, and both sides get weaker.
This matters more in healthcare than in many other categories because the decision is personal and the stakes are high. Patients do not just respond to convenience or price. They respond to confidence, legitimacy, clarity, and the feeling that they are making a safe choice. That is brand territory, even when the final conversion happens through paid search or a provider page.
The practical implication is simple. Healthcare marketing should not ask whether brand or performance matters more. It should ask whether the organization is making the trust layer and the demand layer reinforce each other. When they work together, acquisition becomes more efficient and more resilient.
Local Execution Usually Beats Generic Scale
Healthcare brands often want consistency, and that instinct is understandable. The risk is that consistency turns into centralization so rigid that local realities disappear. A single health system can have major differences in market competition, referral behavior, access capacity, patient demographics, and service-line demand from one region to another.
That means scale has to be smart, not flat. The right model usually combines shared standards with local flexibility. Core brand rules, governance, analytics definitions, provider data standards, and compliance guardrails should stay centralized. Messaging nuance, channel emphasis, local listings, physician visibility, and market-specific priorities should adapt to what is actually happening on the ground.
This is one of the clearest signs that a healthcare marketing function is maturing. It stops confusing control with effectiveness. It starts building systems that are strong enough to scale and flexible enough to stay relevant.
The Biggest Risk Is Optimizing the Wrong Thing
The most dangerous failure in healthcare marketing is not low traffic or weak click-through rate. It is optimizing for numbers that look good while the patient journey gets worse. A team can reduce cost per lead and still attract the wrong demand. It can increase appointment requests and still create more no-shows, more frustration, or more downstream leakage. It can grow fast and still weaken long-term reputation.
That is why expert-level healthcare marketing keeps returning to the same core question: is this making it easier for the right patient to reach the right care with confidence? If the answer is no, the tactic may still produce activity, but it is not producing healthy growth.
That perspective changes how decisions get made. It makes teams more selective about where to automate, where to personalize, where to slow down, and where to push harder. It also prepares the organization for the final step, which is turning everything in this article into a clear operating model and answering the practical questions leaders usually ask when they are ready to act.
Turning Healthcare Marketing Into a Working System
At the end of the day, healthcare marketing works best when it behaves like an operating system, not a collection of disconnected tactics. The strongest organizations connect reputation, provider visibility, patient access, measurement, compliance, and capacity planning so each part reinforces the others instead of creating more friction downstream. That system mindset matters because current consumer behavior keeps pushing healthcare organizations toward easier digital access, stronger trust signals, and better coordination between marketing and operations.
That is also why the final version of healthcare marketing is not just about getting found. It is about building a patient journey that feels credible before the visit, clear during the decision, and consistent after the appointment is booked. When that ecosystem is working, growth becomes easier to sustain because demand is being converted through trust and access rather than brute-force promotion alone.

FAQ
What is healthcare marketing in practical terms?
Healthcare marketing is the discipline of helping the right patients find, trust, and access the right care. In practice, that means combining branding, provider visibility, service-line strategy, digital access, patient education, reviews, and measurement instead of treating each piece like a separate project. The shift toward digital discovery, online scheduling, and provider comparison makes that integrated approach far more important now than it was even a few years ago.
Why does healthcare marketing matter more now than it used to?
Patients have become more active decision-makers, and their expectations are shaped by better digital experiences everywhere else. Research from Press Ganey shows that online scheduling influences provider choice, while Aha Media Group found that provider bios play a major role before booking. That combination means healthcare marketing now shapes demand, trust, and access at the same time.
What makes healthcare marketing different from marketing in other industries?
The biggest difference is that healthcare decisions carry higher stakes, more emotion, and tighter privacy expectations. People are not just comparing convenience or price. They are trying to reduce uncertainty, evaluate credibility, and feel safe sharing sensitive information in a system that can already feel intimidating. Trust and governance therefore matter far more in healthcare marketing than in many standard lead-generation environments.
Which channels matter most in healthcare marketing?
There is no universal channel mix, but search, local listings, provider profiles, reviews, service-line pages, email or SMS follow-up, and scheduling workflows usually matter more than flashy top-of-funnel experiments. Patients often move across several of these surfaces before they act, so channel coordination matters more than raw channel count. Healthcare marketing performs best when every channel supports the same next step instead of forcing the patient to restart the journey each time.
Are reviews really that important in healthcare?
Yes, and not just because they influence reputation in the abstract. Reviews help patients decide whether a provider feels trustworthy, communicative, and worth contacting, especially when they are choosing between similar options. They work best when they are recent, visible, and supported by strong provider pages and consistent access information.
How important are provider profiles and physician bios?
They are much more important than many organizations assume. Aha Media Group’s 2024 research found that 92% of patients read a provider bio before booking, which makes the profile a core decision asset rather than a background content page. In healthcare marketing, a strong bio reduces hesitation, clarifies fit, and helps the patient imagine the real care experience behind the brand.
What should healthcare organizations measure first?
Start with a connected set of metrics rather than a giant reporting deck. The most useful early measures usually include provider profile engagement, review growth, scheduling completion, call connection quality, inquiry-to-appointment conversion, and downstream show rates by service line. Those metrics tell you far more about real healthcare marketing performance than isolated traffic or click metrics ever will.
How should teams think about online scheduling?
Online scheduling should be treated as a trust and access tool, not just a feature. Press Ganey reports that four in five consumers say online scheduling influences provider choice, which means the booking flow is now part of the brand experience. The smart move is not forcing every service into instant scheduling, but making the next step feel obvious and low-friction for each service type.
Does patient portal adoption matter for healthcare marketing?
It does, because portal access is part of the broader digital relationship patients now expect. Federal data from HealthIT.gov show high levels of online record access and stronger portal use when providers actively encourage patients to engage digitally. That means healthcare marketing should not think only about acquisition; it should also support confidence and continuity after the first conversion.
Can AI improve healthcare marketing?
Yes, but only when it is used carefully and within clear governance. AI can help with segmentation, workflow support, content operations, and response speed, but it should not be allowed to weaken accuracy, privacy, or patient trust. In healthcare marketing, AI works best as a controlled support layer inside a strong operating model, not as a shortcut around human review and data discipline.
What are the biggest mistakes healthcare marketing teams make?
A few mistakes show up again and again: overvaluing traffic, underinvesting in provider content, treating access as somebody else’s problem, and scaling campaigns faster than operations can absorb demand. Another common error is separating brand from performance so aggressively that the trust layer and the conversion layer stop reinforcing each other. Those mistakes usually create impressive dashboards and disappointing patient journeys.
How can smaller practices compete with larger systems?
Smaller groups usually win by being clearer, faster, and more specific rather than trying to outspend large systems. A better provider profile, tighter review strategy, stronger local search presence, easier scheduling path, and more human follow-up can create a meaningful edge even without enterprise budgets. In healthcare marketing, operational sharpness often beats scale when the patient is making a high-intent local decision.
How often should a healthcare marketing strategy be reviewed?
The strategy should stay stable longer than the tactics, but the operating data should be reviewed constantly. Most teams benefit from monthly reviews of conversion, access friction, review health, and service-line demand, along with quarterly decisions around budget allocation, channel mix, and capacity alignment. That cadence helps healthcare marketing stay responsive without becoming chaotic or overly reactive.
Work With Professionals
Explore 10K+ Remote Marketing Contracts on MarkeWork.com
Most marketers spend too much time chasing clients, competing on crowded platforms, and losing a percentage of every project to middlemen.
MarkeWork gives you a better way. Browse thousands of remote marketing contracts and connect directly with companies desperate to hire skilled marketers like you, without platform commissions and without unnecessary gatekeepers.
If you're serious about finding better opportunities and keeping 100% of what you earn, explore available contracts and create a profile for free at MarkeWork.com.
