Medical marketing is not regular marketing with a few health words layered on top. It sits in a category where trust, accuracy, privacy, and timing matter more than clever copy, because people are usually searching when they feel uncertain, vulnerable, or pressed for answers. That changes everything from the way a clinic writes website pages to the way it handles reviews, reminders, and follow-up campaigns.
That is why good medical marketing is less about pushing attention and more about removing friction. Patients compare providers online, judge credibility fast, and expect digital experiences that feel clear, helpful, and respectful of their data. At the same time, healthcare organizations have to navigate stricter standards around health claims, endorsements, and the use of tracking tools than most brands ever face.
In practice, medical marketing means building a trustworthy path from first search to first visit and then from first visit to long-term retention. It has to support reputation, education, access, and patient experience all at once. When that system is done well, marketing stops feeling promotional and starts functioning like part of the care journey.
Article Outline
- Why Medical Marketing Matters
- A Practical Framework for Medical Marketing
- The Core Channels That Actually Drive Patient Growth
- Content, Reputation, and Search Authority
- Professional Implementation Inside a Real Practice
- Measuring Results Without Losing Trust
Why Medical Marketing Matters
Medical marketing matters because the patient journey now starts long before a phone call. People research symptoms, compare providers, read reviews, scan bios, and check whether a practice feels credible before they ever book. In healthcare, that early impression is not just a branding issue. It directly affects whether a patient feels safe enough to take the next step.
It also matters because healthcare is one of the toughest categories to market responsibly. The HIPAA Privacy Rule limits how protected health information can be used for marketing, and HHS has also issued specific guidance on online tracking technologies used on regulated health websites and apps. Add FTC standards for scientific substantiation and endorsements, and you get a field where sloppy growth tactics can quickly become a compliance problem.
Then there is the platform layer. Health content lives in a high-scrutiny environment because search systems and evaluators treat medical topics as the kind of information that can affect a person’s health, safety, or financial stability. That means weak content, anonymous expertise, and thin pages are a much bigger liability in medical marketing than they are in lighter niches.
The practical takeaway is simple: medical marketing has to earn attention instead of buying it cheaply. A practice that communicates clearly, proves expertise, protects privacy, and makes access easier will usually outperform a louder competitor with a weaker patient experience. That is why the best strategy starts with trust architecture, not campaign hacks.
A Practical Framework for Medical Marketing
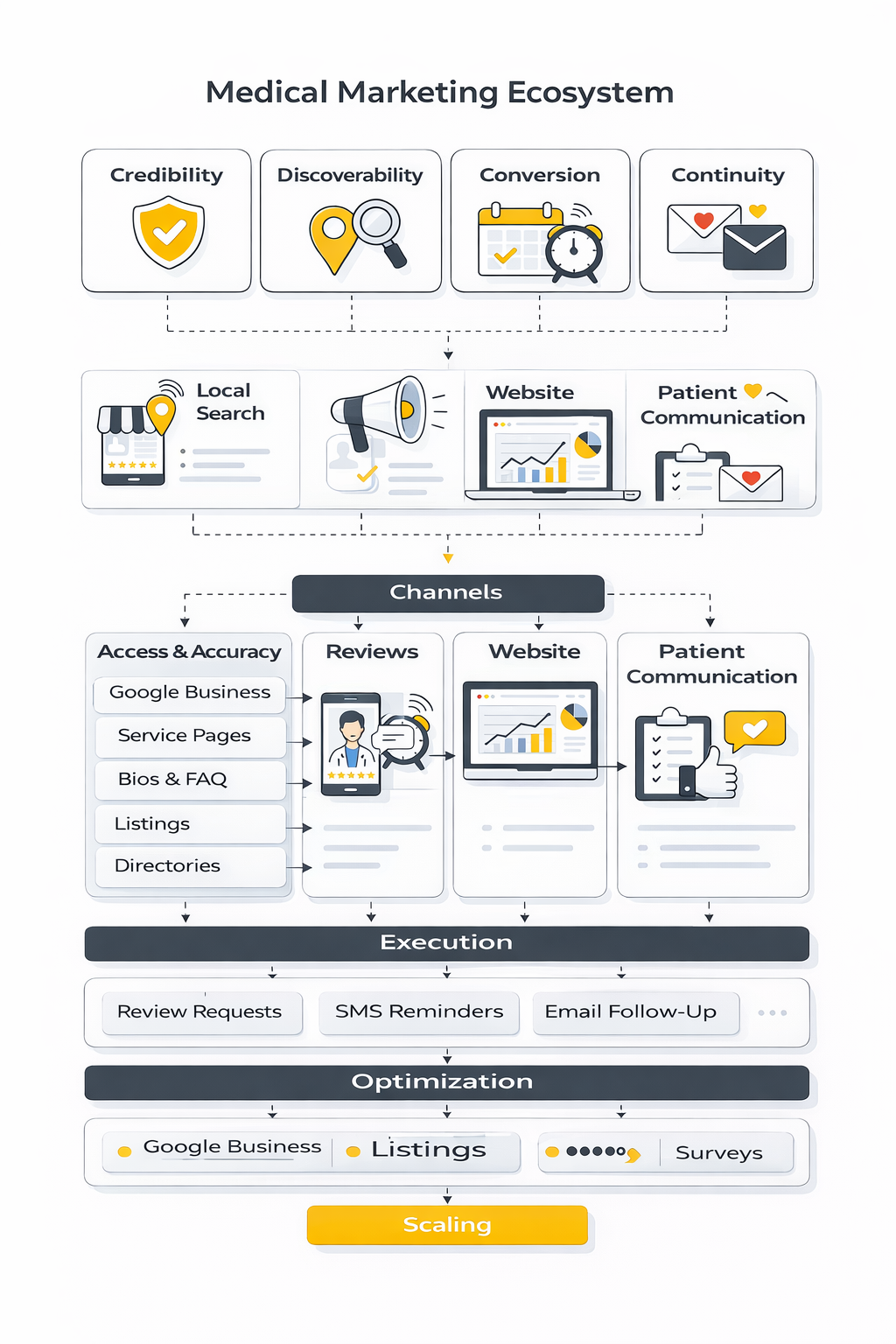
The cleanest way to think about medical marketing is as a four-part system: credibility, discoverability, conversion, and continuity. Credibility answers why a patient should trust you. Discoverability makes sure the right people can find you. Conversion helps them book without confusion. Continuity keeps the relationship active after the first visit so retention and referrals can grow naturally.
That framework works because it matches real patient behavior better than a channel-first approach. Most practices make the mistake of asking whether they need SEO, paid ads, social media, or email, when the better question is where trust is breaking down in the patient journey. Once that is clear, the channel mix becomes much easier to choose and much easier to measure.
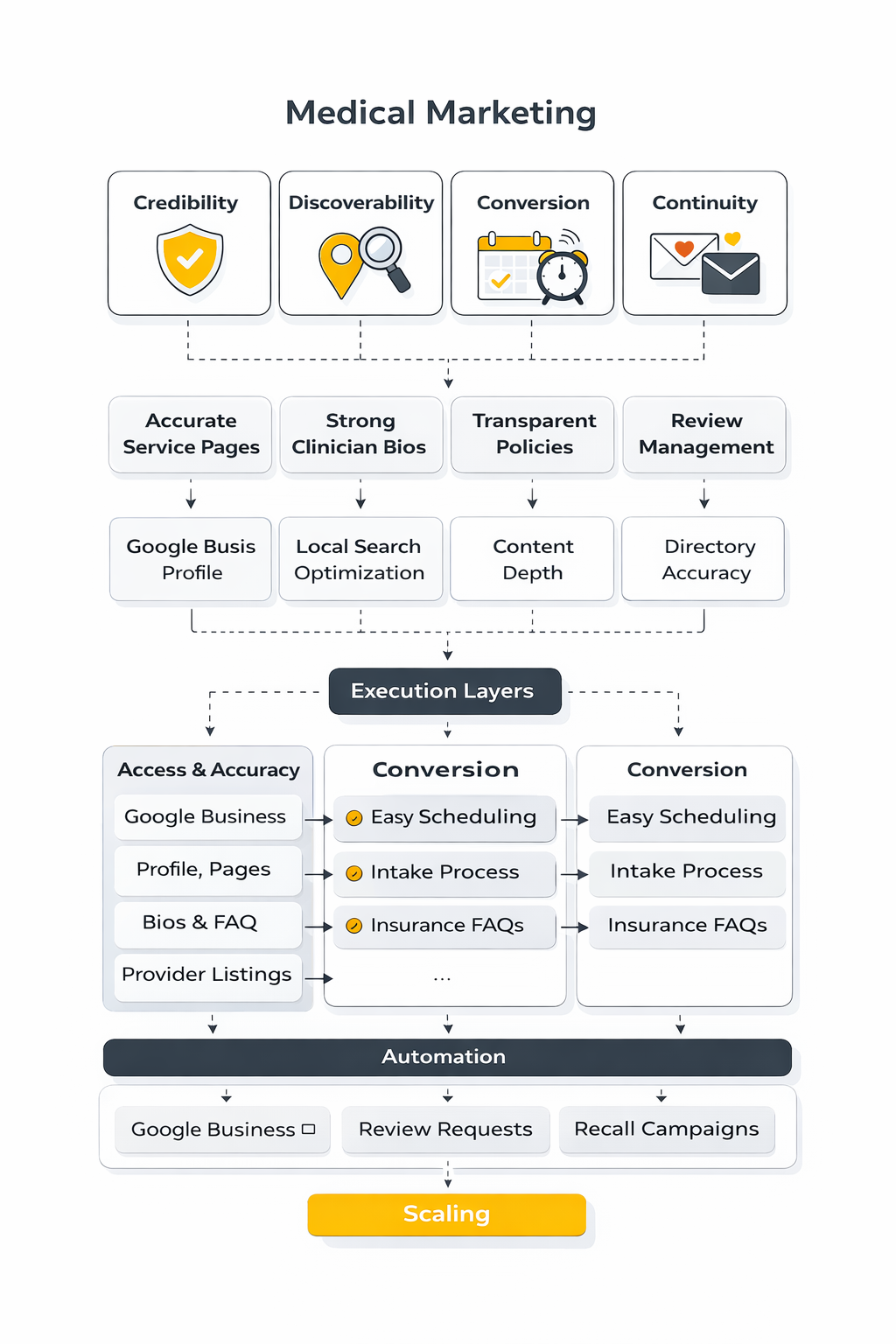
Credibility comes first because every later tactic depends on it. In medical marketing, credibility usually shows up through accurate service pages, strong clinician bios, transparent policies, review management, educational content, and a site experience that feels professional instead of vague or promotional. Even a strong ad campaign struggles if the landing experience feels generic, outdated, or evasive.
Discoverability is the second layer. This is where local search visibility, specialty pages, referral pathways, directory accuracy, and content depth matter. Search visibility in healthcare is rarely won by publishing random blog posts. It is won by building a clear structure around patient intent, clinical expertise, and location relevance.
Conversion is where many practices lose momentum. A patient may be fully convinced and still drop off because the forms are clunky, scheduling is unclear, insurance information is buried, or there is no practical next step after reading a page. This is the point where operational tools, including systems like GoHighLevel, can be useful when they are configured around patient communication workflows rather than generic lead generation.
Continuity is what turns marketing from a cost center into a growth system. Follow-up education, appointment reminders, recall campaigns, reputation requests, and patient-friendly communication can strengthen retention when they are handled in a compliant and thoughtful way. The point is not to automate everything. The point is to make it easier for patients to stay engaged without feeling marketed to.
The Core Channels That Actually Drive Patient Growth
A lot of medical marketing plans get bloated because they treat every channel like a must-have. In reality, most practices grow from a smaller set of channels that match how patients actually choose care: local search, reputation, the website, and patient communication. When those four work together, the rest of the strategy gets easier to scale and much easier to measure.
The important shift is this: patients are not moving through a neat funnel. They bounce between Google results, maps, reviews, physician bios, insurance details, and scheduling pages before they decide. That is why the strongest medical marketing systems are built around decision moments, not around whatever platform feels trendy this quarter.
Local Search Is Usually the First Battleground
For many practices, local search is where visibility either starts or dies. A Google Business Profile with accurate categories, services, hours, photos, messaging, and booking links is not a side task anymore. Google’s own 2026 Business Profile playbook highlights that complete profiles earn more clicks, reviews influence decisions, and 77% of consumers expect to be able to book services online.
This matters even more in medical marketing because patients often search with local intent even when they do not type a city. They look for terms like urgent care, dermatologist, physical therapist, or pediatric dentist and then filter fast based on location, ratings, and convenience. If your profile is incomplete or your service information is vague, you are forcing patients to keep looking.
The practical lesson is not complicated. Claim the profile, choose precise categories, keep hours updated, add real photos, list services clearly, and make the booking path obvious. None of that feels glamorous, but it directly affects discoverability and trust at the exact moment a patient is deciding.
Reviews Carry More Weight Than Most Practices Realize
Reviews are not just a reputation layer anymore. They are part of the discovery engine itself, because patients often compare ratings before they even visit a website. Google’s current guidance points out that reviews build trust and visibility, while recent consumer research shows 91% of consumers use reviews to evaluate local businesses and 65% are more likely to choose a business that responds to reviews.
Healthcare adds another layer of intensity because trust is personal. In a recent patient preference report, 40% of patients said they had canceled an appointment or changed a care plan based solely on online reviews. That is a massive signal that reviews are not just social proof in medical marketing. They are part of care selection itself.
The smartest response is not to chase vanity ratings. It is to create a review process that is ethical, consistent, and operationally easy for staff to support. Ask at the right moment, make it simple, respond professionally, and use feedback to fix real issues instead of treating reviews like a cosmetic exercise.
Your Website Has to Reduce Friction, Not Add More
A healthcare website should answer the practical questions patients are already carrying into the search. Can this practice help with my issue, do they take my insurance, who will I see, where are they located, and how do I book without calling three times. When those answers are buried, even strong traffic turns into wasted demand.
That is why access information has become a marketing issue, not just an operations issue. In Press Ganey’s recent consumer research, 49% of patients said accurate and relevant information online influenced provider choice, and 43% said the ability to schedule or reschedule online mattered. Medical marketing works better when the website feels like a front door, not like a brochure.
This is also where many practices underinvest. They spend on traffic before fixing clinician bios, service pages, FAQs, scheduling steps, or mobile usability. That is backward. Better conversion usually starts with clearer information and fewer clicks, not with more ad spend.
Online Scheduling Is No Longer Optional for Growth-Focused Practices
Online scheduling has moved from nice-to-have to baseline expectation. Patients do not compare your booking flow to other clinics only. They compare it to every modern digital experience they use every week. That is a brutal standard, but it is the one that now shapes patient behavior.
Recent healthcare consumer data shows the demand is broad, not limited to younger audiences. Press Ganey found that 81% of people ages 45 to 60 and 85% of those ages 30 to 44 say online scheduling influences provider choice. Google’s latest Business Profile material reinforces the same point from another angle by showing strong consumer expectations for online booking directly from local business listings.
This is where the right system matters. If a practice is coordinating reminders, follow-ups, intake prompts, and rebooking workflows, a platform such as GoHighLevel can be useful when it is set up carefully around patient communication rather than generic lead funnels. The key is to simplify access without creating privacy or messaging problems in the process.
Patient Communication Is a Growth Channel Too
A lot of practices still separate marketing from communication, and that creates avoidable drop-off. The reminder that prevents a no-show, the follow-up that helps a patient return, and the message that prompts a review request are all part of medical marketing when they support trust and continuity. Growth is often won in those quiet moments after the first conversion.
There is also a strong convenience signal here. Google’s Business Profile playbook cites messaging preference data showing that 67% of people prefer messaging a business to a call or email. That does not mean every practice should turn into a chat-first business, but it does mean patients increasingly expect fast, low-friction contact options.
The warning is obvious and important. In healthcare, convenience cannot outrun compliance. HHS has continued to stress the risks around online tracking technologies on regulated health websites and apps, so every communication workflow needs to be built with privacy in mind from the start.
Content, Reputation, and Search Authority
Once the core channels are in place, medical marketing needs authority signals that compound over time. That is where content, reputation, and search quality start reinforcing each other. A practice with strong pages, strong reviews, and clear expertise will usually outperform a competitor that tries to manufacture trust through ads alone.
This matters more in healthcare than in lighter categories because medical topics sit in a high-stakes information environment. Search systems evaluate trust signals closely when content can influence health decisions, which means thin pages, weak authorship, and vague expertise become expensive problems over time. Good authority is earned through clarity, depth, and credibility, not through publishing volume for its own sake.
Educational Content Has to Be Useful Before It Can Be Persuasive
The best healthcare content does not read like a pitch. It answers the questions patients actually have before, during, and after treatment decisions. That includes symptoms, treatment options, risks, timelines, candidacy, cost context, recovery expectations, and what happens next.
This is where a lot of medical marketing content fails. It chases keywords without matching patient intent, so the page ranks poorly, converts poorly, or both. Useful content works better because it reduces uncertainty, and uncertainty is often the biggest blocker between interest and appointment.
Google’s guidance on helpful, people-first content is especially relevant here. In healthcare, usefulness is not just an SEO principle. It is the difference between content that builds trust and content that makes a practice look careless.
Reputation and Content Should Support Each Other
Strong reviews without strong content leave gaps. Strong content without a visible reputation leaves doubt. The real win in medical marketing comes when a patient finds a service page, checks the clinician profile, sees consistent patient feedback, and feels that the entire experience lines up.
That alignment is what creates search authority in practice. A detailed service page can explain the treatment. Reviews can validate the experience. A complete local profile can confirm access details. Together, those elements create confidence that is much harder for a competitor to copy than a paid campaign or a prettier homepage.
The next step is implementation. Once a practice understands the right channels and the right authority signals, the real question becomes how to build the system without overwhelming the team or creating compliance risk.
Professional Implementation Inside a Real Practice
This is the point where medical marketing stops being a strategy deck and becomes an operating system. Most practices do not fail because they picked the wrong channel. They fail because nobody owns the full patient journey from discovery to booking to follow-up, so the experience breaks in small places that quietly kill growth.
That is why implementation has to be cross-functional from day one. Marketing, front desk, operations, compliance, and clinical leadership all influence whether the patient experience feels trustworthy and easy. In healthcare, a campaign can work on paper and still fail in reality because wait times are too long, scheduling rules are too confusing, or online information is not aligned with what staff say on the phone.
A useful way to roll out medical marketing is to build it in layers. Start with access and accuracy, then strengthen conversion, then automate carefully, and only then add scale channels. That order matters because more traffic does not fix a weak patient experience. It only sends more people into it.
Start With Access, Accuracy, and Ownership
The first job is not content production or ad buying. It is making sure the basics are true, current, and easy to manage. That means service pages, clinician bios, locations, hours, insurance details, provider listings, and booking pathways all need a clear owner inside the practice.
This sounds almost too basic, but it is where a huge amount of leakage happens. CMS has repeatedly emphasized that accurate provider directory information is critical for patients trying to find care that fits their needs, and the agency is still pushing broader efforts to improve directory quality and reduce fragmentation across the system through initiatives like the National Directory of Healthcare Providers & Services effort. If your own site, your profiles, and your third-party listings disagree, trust starts breaking before the first visit.
The same principle applies internally. One person should own website updates, one person should own local profiles, and one person should own reporting. Medical marketing gets messy when everything belongs to everyone and therefore nothing gets fixed quickly.
Build the Patient Journey Backward From the Appointment
Once the fundamentals are accurate, the next move is to map the journey backward from the booked appointment. Start with the conversion point and ask what a patient needs to believe, understand, and complete before they get there. That gives you a much cleaner implementation plan than starting with content topics or ad ideas.
For most practices, that journey has five obvious checkpoints:
- The patient finds the practice.
- The patient trusts what they see.
- The patient confirms the practice fits their need.
- The patient books without friction.
- The patient actually shows up and stays engaged.
That last point matters more than many teams admit. Missed appointments are not just an operations problem. They are also a patient communication problem, a reminder problem, and sometimes an access problem. Newer research continues to show that reminders and communication workflows improve attendance, including a 2026 study where attendance was higher among patients who confirmed receiving SMS reminders and broader 2025 to 2026 evidence reviews linking reminders to lower no-show rates and better continuity of care through studies like this analysis of missed appointments.
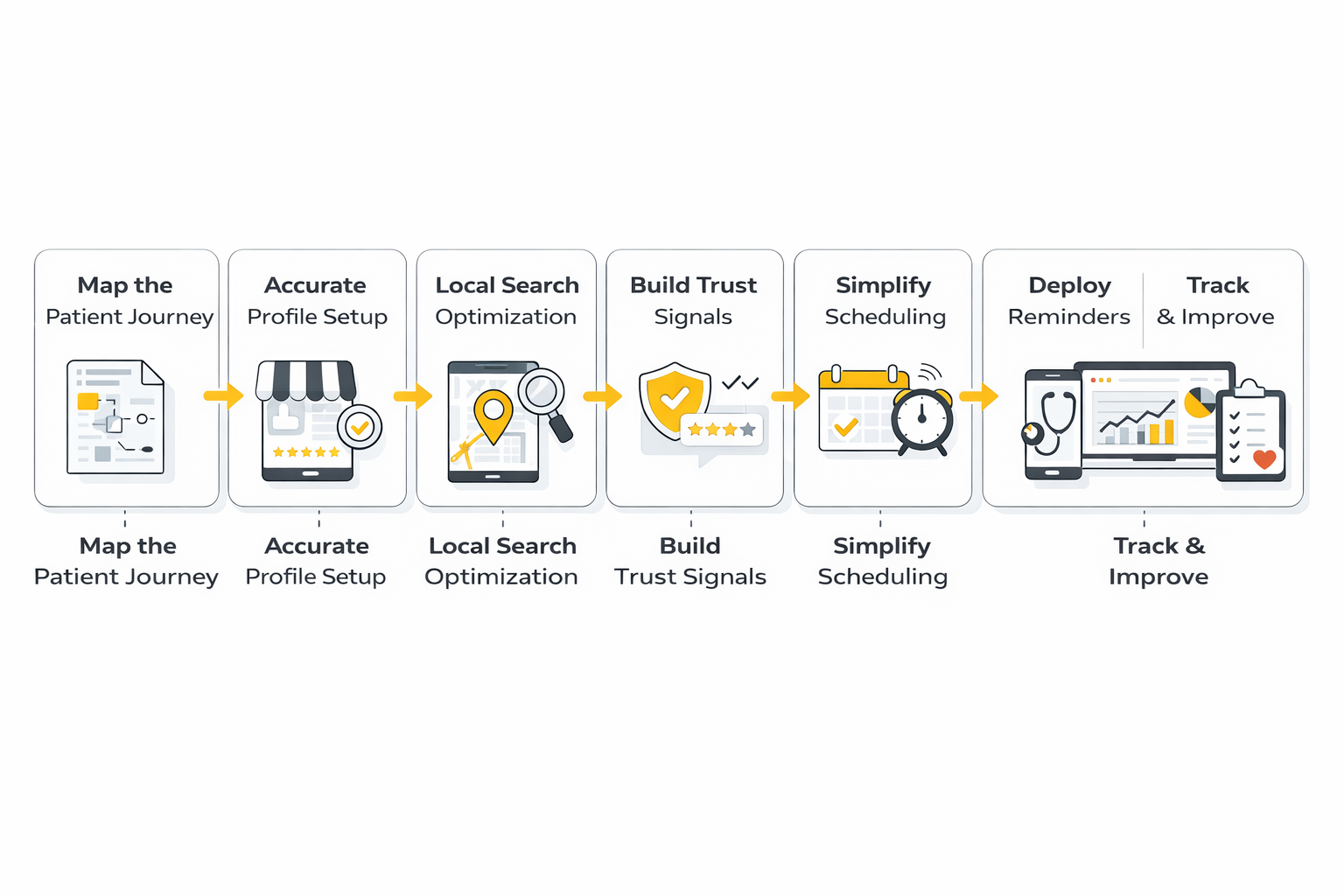
When you make this process visible, execution gets much easier. You can assign one page, one workflow, and one owner to each stage instead of talking about growth in vague terms. That is how medical marketing becomes operational instead of aspirational.
Use a Simple Rollout Sequence
Most practices do better with a phased rollout than a full rebuild. The first phase should fix trust and access blockers. The second should improve scheduling and follow-up. The third should expand content and traffic sources once conversion is stable.
A practical sequence usually looks like this:
- Audit profiles, listings, service pages, bios, and contact paths.
- Fix booking friction on the website and Google Business Profile.
- Standardize intake, reminders, and review requests.
- Build high-intent service and location pages.
- Add paid acquisition only after conversion data is clean.
This order lines up with how patients behave today. McKinsey’s work on digital transformation shows health systems continue prioritizing digital front doors because they affect scheduling, navigation, education, payment, and ongoing care management in one connected layer, with about 70% of respondents expecting the highest impact from virtual health and digital front door investments. In other words, access is not a support feature anymore. It is part of the growth engine.
Keep Compliance Inside the Workflow, Not at the End
This is where a lot of otherwise smart teams get sloppy. They build forms, trackers, automations, or retargeting campaigns first and then ask whether the setup is compliant. In medical marketing, that order is dangerous.
HHS remains very clear that HIPAA places boundaries around what counts as marketing and when authorization may be required, especially when communications encourage use of a product or service outside the rule’s exceptions in the agency’s marketing guidance. HHS has also kept the pressure on organizations using online tracking technologies on regulated health websites and apps, which means implementation decisions around pixels, analytics, forms, and chat tools should be reviewed before launch, not after complaints start.
The practical move is simple: compliance review should be part of the build checklist. Every form, reminder flow, chatbot, analytics setup, review workflow, and messaging tool should be assessed before it goes live. That sounds stricter, but it actually speeds execution because the team stops rebuilding the same system twice.
Make Scheduling and Pre-Visit Preparation Part of Marketing
A lot of teams still think marketing ends when the appointment is booked. In medical marketing, that is too narrow. The handoff between scheduling and care delivery shapes whether the patient follows through, how prepared the visit is, and whether the relationship continues.
That is why pre-visit communication matters. AMA guidance on pre-visit planning shows that structured preparation can save time, improve visit quality, and reduce follow-up calls and portal messages. From a growth perspective, that means better throughput, fewer avoidable frustrations, and a smoother experience that patients are more likely to review positively and recommend.
This is also where automation can help if it is used with discipline. A platform such as GoHighLevel can support reminders, lead routing, intake prompts, and follow-up sequences, but the setup has to reflect healthcare reality. The winning version is the one that reduces friction for patients and admin load for staff without creating messaging chaos.
Train the Front Desk Like Part of the Growth Team
This point gets missed constantly. Front-desk performance is one of the biggest hidden variables in medical marketing because it affects conversions that never show up cleanly in ad dashboards. A practice can rank well, earn clicks, and still lose patients because phone handling is inconsistent or scheduling answers are unclear.
That is especially costly right now because access pressure is not easing. MGMA highlighted 2025 data showing the average wait time for a new-patient appointment had risen to 31 days, up 19% since 2022. When access is tight, every avoidable missed call, confused handoff, or delayed response hurts more.
The fix is operational, not theoretical. Give staff scripts for common questions, define escalation rules, standardize how insurance and availability are explained, and review missed-call patterns every week. In a strong medical marketing system, the front desk is not downstream from growth. It is part of growth.
Document the Process Before You Try to Scale It
The practices that scale best are usually not the flashiest. They are the ones that document what happens when a patient fills out a form, calls after hours, requests a consult, misses an appointment, leaves a review, or goes quiet for six months. That documentation turns good intentions into repeatable execution.
This matters because growth breaks under variability. If one staff member sends review requests, another forgets, and a third uses different wording every time, the system becomes impossible to optimize. The same is true for intake, reactivation, referral follow-up, and scheduling callbacks.
A lightweight playbook is enough at the beginning. Write the triggers, the owner, the timing, the channel, and the exception cases. Once that exists, medical marketing becomes measurable because the practice can finally tell the difference between a strategy problem and an execution problem.
Measuring What Actually Matters in Medical Marketing
Most medical marketing dashboards look impressive and still fail to answer the only question that matters: are more qualified patients finding you, booking, showing up, and staying? That gap between activity and outcomes is where a lot of practices get stuck.
The issue is not lack of data. It is too much disconnected data. Website analytics, call tracking, scheduling systems, reviews, and EHR data all live in different places, so teams end up optimizing for what is easiest to see instead of what actually drives growth.
The fix is to simplify measurement around the patient journey you already mapped. Every metric should connect to one of those five stages: find, trust, confirm, book, and show up. If it does not clearly support one of those steps, it is probably noise.
The Only Metrics That Deserve Daily Attention
You do not need 40 KPIs to run effective medical marketing. You need a short list that reflects real patient behavior. The strongest practices usually track a tight group of signals and review them consistently instead of chasing every available report.
At a minimum, focus on:
- Search visibility for core services and locations
- Click-through rate from search to website or profile
- Conversion rate from visitor to booked appointment
- Call answer rate and missed-call recovery
- Appointment show rate
- Review volume and average rating trend
Each of these metrics ties directly to revenue and patient experience. For example, a high ranking with a low click-through rate usually signals weak titles, poor reviews, or unclear positioning. A strong conversion rate with a low show rate points to communication or reminder problems, not marketing problems.
This is where interpretation matters more than the number itself. Metrics only become useful when they tell you what to fix next.
Benchmarks Mean Less Than You Think, Direction Means More
Healthcare marketers often ask for benchmark conversion rates or average costs per patient. Those numbers can be helpful for context, but they are dangerous when used blindly. Medical marketing varies too much by specialty, location, payer mix, and patient urgency for a single benchmark to guide decisions.
What matters more is trend direction. If your booking rate improves after simplifying your scheduling page, that is a meaningful signal. If your show rate increases after implementing SMS reminders, that is actionable progress.
There are still some directional patterns worth understanding. Press Ganey’s recent data shows how strongly access influences patient choice, with large segments of patients prioritizing convenience features like online scheduling and accurate information. That reinforces the idea that improvements in access and communication often outperform pure traffic growth in medical marketing.
Build a Simple Analytics System That Matches Reality
The goal is not to build a perfect attribution model. In healthcare, perfect attribution is almost impossible because patients move between online and offline touchpoints. The goal is to build a system that is simple enough to trust and detailed enough to guide action.
A practical setup usually includes:
- Website analytics for traffic and behavior
- Call tracking for inbound phone performance
- Scheduling data for conversion and attendance
- Review monitoring for reputation trends
- A basic CRM layer to connect interactions over time
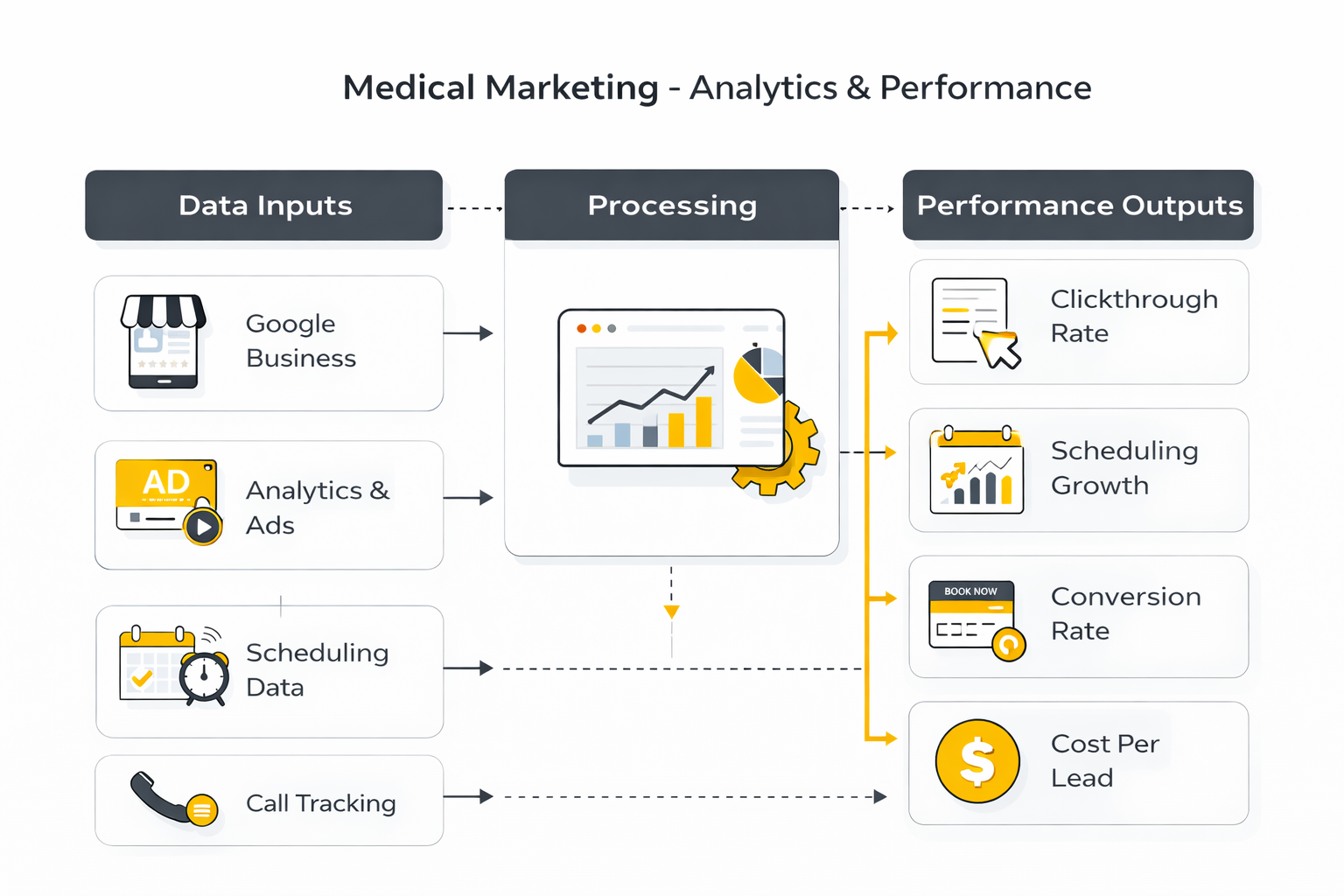
When these pieces are connected, patterns start to emerge quickly. You can see which services drive calls, which pages convert, which campaigns bring low-quality leads, and where patients drop off. That is when medical marketing becomes predictable instead of reactive.
Tools can help here, but only if they are configured around the patient journey. A platform like GoHighLevel can centralize leads, calls, messages, and follow-ups, which makes it easier to see what happens between first click and final appointment. The value is not the tool itself. The value is having one place where the journey is visible.
Understand What the Data Is Really Telling You
Data in medical marketing rarely points to a single isolated problem. It usually highlights a system issue. The mistake is to treat symptoms instead of causes.
For example:
- High traffic + low bookings often means unclear services or weak trust signals
- High bookings + low show rate usually means poor reminders or long wait times
- Strong reviews + low traffic suggests a discoverability problem, not a reputation problem
- High call volume + low answer rate points to staffing or process gaps, not demand issues
This is where many practices misallocate budget. They increase ad spend to fix what is actually a conversion or operations issue. That approach almost always leads to higher costs without better results.
The better move is to follow the signal backward. If patients are dropping off at a specific step, fix that step first before scaling anything upstream.
Use Data to Decide What Not to Do
One of the most valuable outcomes of good measurement is clarity on what to ignore. Medical marketing becomes much easier when you stop investing in channels or tactics that do not move core metrics.
If social media engagement is high but bookings do not change, it may not deserve more budget. If a paid campaign drives traffic but not qualified patients, it needs to be reworked or paused. If a service page ranks but does not convert, the issue is probably clarity, not visibility.
This discipline protects both budget and team focus. It also keeps the strategy aligned with patient outcomes instead of vanity metrics.
Keep Measurement Close to the Team That Executes
The final piece is cultural, not technical. Data should not live in monthly reports that nobody uses. It should be part of weekly conversations between marketing, front desk, and leadership.
When the team reviews missed calls, booking rates, and no-shows together, patterns become obvious faster. Small fixes get implemented quicker. And medical marketing starts behaving like a feedback system instead of a one-way campaign engine.
That shift is subtle, but it changes everything.
Strategic Tradeoffs, Risks, and What Happens When You Scale
Once the basics are working, medical marketing gets harder in a more interesting way. The challenge is no longer just getting found. The challenge is scaling growth without damaging trust, overloading staff, or creating compliance problems that quietly erase the gains.
That is where a lot of practices make the wrong move. They assume the next stage is simply more content, more ads, or more automation. In reality, the next stage is usually better coordination between marketing, access, operations, and governance.
Growth Can Outrun Capacity Faster Than You Think
One of the biggest traps in medical marketing is solving demand before solving capacity. If your campaigns work but your schedule is already tight, the patient experience can deteriorate quickly. Long waits, missed callbacks, and appointment bottlenecks turn good marketing into a reputation risk.
That problem is not theoretical. Recent healthcare access analysis from McKinsey argues that access challenges are now structural and require changes across care models, operations, and digital pathways rather than isolated fixes. In plain English, demand generation without access redesign eventually creates frustration instead of growth.
This is why advanced medical marketing has to be capacity-aware. Before scaling acquisition, a practice should know which services have room, which providers are constrained, and which patient types are creating the highest operational load. That prevents the common mistake of marketing everything equally when the business can only support some of it well.
AI Can Improve the Experience, but It Can Also Flatten Trust
AI is going to reshape medical marketing, but not every use case deserves the same enthusiasm. Used well, it can help with intake, routing, scheduling support, content operations, and personalization. Used badly, it produces generic health content, awkward automation, and patient interactions that feel cold at exactly the moment reassurance matters most.
That tension is becoming more important as healthcare organizations push digital experience improvements. Newer work from McKinsey on AI-powered healthcare consumer experiences makes the case that trust and human-centered design still sit at the center of adoption, even when AI is part of the solution. That matters because in medical marketing, efficiency is never the only goal.
The smart play is selective use. Let AI support structured tasks, triage, and operational speed. Do not let it replace clinical nuance, careful claims review, or the voice that patients rely on when decisions feel serious.
Claims, Testimonials, and Positioning Need More Discipline at Scale
As a practice grows, brand pressure grows with it. Teams want stronger headlines, sharper promises, and more aggressive conversion copy. That is exactly when marketing discipline matters most.
The FTC’s health claims guidance makes the standard clear: health-related claims need solid substantiation, and that expectation is higher, not lower, when a message could influence medical decisions. In healthcare, that means vague superlatives, oversimplified outcomes, and loosely framed testimonial language can create more downside than upside.
This gets especially important when multiple locations, providers, or agencies are involved. A claim that sounds harmless in one ad can become risky when repeated across landing pages, videos, social posts, and review prompts. Advanced medical marketing requires a claims review mindset, not just a copywriting mindset.
Attribution Gets Messier as the Organization Gets Bigger
Small practices can sometimes get away with simple channel tracking. Larger groups cannot. Once you add multiple locations, provider specialties, call centers, referral patterns, and longer decision cycles, attribution becomes less clean and more political.
That is why expert-level medical marketing focuses less on perfect attribution and more on decision-grade attribution. You need enough visibility to know what is driving qualified demand, where friction is increasing, and which investments are creating operational strain. You do not need a fantasy dashboard that pretends every patient journey is linear.
This is also the stage where CRM and workflow tooling start mattering more. A system like GoHighLevel can help centralize inquiries, follow-ups, and pipeline visibility, but the real advantage comes from process design, not software alone. If the team lacks naming conventions, source rules, and ownership, the platform will simply help them get confused faster.
Privacy Risk Increases With Every New Tool You Add
Scaling usually means adding more vendors, more tracking, more forms, and more workflow layers. That also means more privacy exposure. In medical marketing, every new tool should be treated like a governance decision, not just a feature upgrade.
That caution is still warranted given the ongoing focus from HHS on HIPAA guidance materials and online tracking technologies. Even where legal interpretation has shifted over the past two years, the practical message for healthcare operators is the same: know what data is collected, where it flows, who receives it, and whether that setup fits the actual risk profile of your organization.
This is where advanced teams separate themselves. They do not bolt privacy checks onto the end of execution. They build vendor review, form review, and data-flow review into the marketing process itself.
Brand Consistency Becomes Harder Across Locations and Providers
A single-location practice can keep brand quality tight through direct oversight. A multi-location group cannot rely on that forever. Once multiple people are updating bios, requesting reviews, answering calls, writing pages, and handling inquiries, inconsistency starts creeping in fast.
That inconsistency hurts more in medical marketing than in many other industries because patients are trying to assess reliability. If one location looks polished and responsive while another looks outdated and disorganized, the entire brand starts to feel less dependable. Trust does not fragment neatly by office. Patients usually generalize.
The fix is not to make every page sound robotic. It is to define what must stay consistent: claims standards, response standards, provider bio structure, review workflows, scheduling language, and core service positioning. That is how a healthcare brand scales without becoming uneven.
The Best Practices Usually Win by Narrowing Focus
At a certain point, strategic restraint becomes a competitive advantage. Strong medical marketing is not about doing everything that is available. It is about doing the few things that compound: clearer positioning, stronger service pages, smoother access, better review systems, better follow-up, and cleaner measurement.
That may sound less exciting than chasing every new tactic, but it is usually what scales. Healthcare is a trust-heavy market with operational constraints. Focused execution tends to beat clever experimentation when patients are making serious decisions.
That is also what separates serious growth from noisy activity. The best teams know where they are different, where they are credible, and where the patient journey still breaks. Then they keep tightening those points until the system becomes hard to compete with.
Before you scale further, it helps to see medical marketing as one connected system rather than a stack of isolated tactics. Search visibility, reviews, website clarity, scheduling, reminders, analytics, staff training, and compliance all influence each other. That is why the strongest practices stop thinking in campaigns and start thinking in systems.
A practice with average ads but a clean patient journey will usually outperform a practice with aggressive promotion and broken follow-through. That may not sound flashy, but it is how sustainable growth actually works in healthcare. When trust, access, and measurement stay aligned, medical marketing becomes more resilient and much easier to improve over time.
FAQ
What is medical marketing, exactly?
Medical marketing is the process of helping patients find, evaluate, trust, and choose a healthcare provider or service. It includes local search visibility, websites, reviews, educational content, patient communication, scheduling, and retention. The difference from general marketing is that healthcare decisions happen in a high-trust, high-sensitivity environment shaped by privacy rules, reputation signals, and clinical credibility.
Why is medical marketing different from normal digital marketing?
The biggest difference is that patients are not casual buyers. They are often stressed, uncertain, and trying to make decisions with real health consequences, which means accuracy and trust matter more than clever messaging. Healthcare organizations also operate under stricter privacy and advertising expectations through rules and guidance from HHS and the FTC.
What channels matter most in medical marketing?
For most practices, the highest-impact channels are local search, reviews, the website, online scheduling, and patient communication workflows. Those channels shape the real decision path far more consistently than vanity-heavy social campaigns. Paid ads can help, but they tend to work best after discoverability, trust, and conversion basics are already in place.
Is SEO still important for medical marketing?
Yes, but not in the shallow way many agencies sell it. Medical SEO is less about publishing endless blog posts and more about building strong service pages, location relevance, clinician credibility, structured site architecture, and useful content that matches patient intent. Search guidance around helpful content from Google Search Central matters here because healthcare pages are judged more critically than low-stakes topics.
How important are online reviews for medical practices?
They are extremely important because reviews influence both visibility and trust. Patients often compare providers before they ever visit a website, and review quality shapes whether a practice feels safe, responsive, and credible. Current healthcare-focused review research from rater8 and RepuGen shows the same basic pattern: patients rely heavily on online feedback when choosing care.
Should every medical practice offer online scheduling?
Not every practice needs the same type of scheduling flow, but most growth-focused practices need some form of online booking or request capability. Patients increasingly expect to move forward without long hold times or back-and-forth friction, and that expectation now affects provider choice. If fully open scheduling is not realistic, then a guided request form, triage flow, or assisted booking process is usually a better answer than forcing everyone to call.
What should a medical practice measure first?
Start with the metrics tied directly to the patient journey: visibility, click-through rate, inquiry volume, booking rate, show rate, and review trend. Those numbers tell you whether patients can find you, trust you, act, and follow through. If you measure only traffic or impressions, you can easily mistake activity for progress.
How do you know whether a medical marketing strategy is actually working?
A good strategy creates improvement across connected outcomes, not just one dashboard widget. You should see stronger visibility for the right services, more qualified inquiries, smoother booking, better attendance, and more stable retention or reactivation. When multiple signals improve together, that usually means the system is healthier rather than one channel temporarily spiking.
Can automation help in medical marketing, or does it make things worse?
Automation can absolutely help, but only when it reduces friction without making communication feel careless. Reminders, follow-ups, intake prompts, review requests, and routing workflows are all strong use cases when they are configured with privacy and timing in mind. The danger is not automation itself. The danger is automating broken processes or sending messages that feel generic in a setting where trust matters.
What are the biggest mistakes practices make with medical marketing?
One common mistake is scaling traffic before fixing access and conversion. Another is treating compliance as a last-minute review instead of a build requirement, especially with forms, tracking tools, and messaging systems discussed in HHS guidance materials. A third is separating marketing from operations, even though front-desk handling, scheduling speed, and reminder quality directly affect results.
Is social media necessary for every healthcare provider?
Not always. Social media can help with awareness, credibility, and education, but it is rarely the first lever that fixes patient acquisition for local practices. If a practice has weak reviews, unclear service pages, or poor booking flow, social content will not solve the underlying problem.
How should medical practices think about AI in marketing?
AI should support structured work, not replace judgment. It can help with content workflows, intake assistance, summarization, routing, and operational speed, but healthcare messaging still needs human review, claims discipline, and empathy. The right question is not whether to use AI. It is where AI improves the patient experience without weakening trust.
What does a strong medical marketing system look like after six to twelve months?
It usually looks calmer, not louder. The practice has cleaner positioning, stronger service pages, more consistent reviews, better scheduling flow, clearer reporting, and tighter coordination between marketing and operations. That is the real sign of maturity in medical marketing: fewer random tactics, better patient movement, and a system the team can actually manage.
Work With Professionals
Explore 10K+ Remote Marketing Contracts on MarkeWork.com
Most marketers spend too much time chasing clients, competing on crowded platforms, and losing a percentage of every project to middlemen.
MarkeWork gives you a better way. Browse thousands of remote marketing contracts and connect directly with companies desperate to hire skilled marketers like you, without platform commissions and without unnecessary gatekeepers.
If you're serious about finding better opportunities and keeping 100% of what you earn, explore available contracts and create a profile for free at MarkeWork.com.
